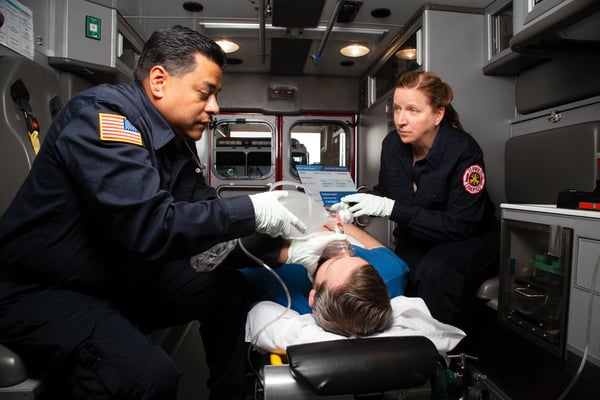
How EMS Technology Integration Can Have Compounding Value for Agencies
Guarantee Your ePCR Works For You, Not Against You: Part 1
We asked Steven Cohen, the Assistant Director of EMS at the Jersey City Medical Center EMS Department in New Jersey, about how their ePCR system helps them achieve their patient care mission of providing great care, while accommodating changing local and national requirements

We asked Steven Cohen, the Assistant Director of EMS at the Jersey City Medical Center EMS Department in New Jersey, about how their ePCR system helps them achieve their patient care mission of providing great care, while accommodating changing local and national requirements. In part one of this three-part series, we asked Cohen to discuss how key performance indicators (KPIs) allow agencies to make sure they are in line with their community, state and national standards for excellence in pre-hospital care.
ZOLL: What are the key KPIs for an EMS service to measure?
Cohen: As I’m sure you have heard from your colleagues, “if you’ve seen one EMS system, you’ve seen one EMS system.” They’re all different. What’s important for me to measure and to capture in my system in our urban setting may not be the same as what somebody wants to capture and measure anywhere out in middle America.
ZOLL: Even though the KPIs may vary, are there any steps that each EMS service, regardless if they are urban or rural, should take?
Cohen: The first step is to collect data. In order to collect the data that you need about your service, the data collection tool – or the electronic Patient Care Reporting (ePCR) system – must be customizable to your needs.
You want the ability to collect data in addition to the minimum data required by your state or the National EMS Information System (NEMSIS). There are a ton of requirements that you have to meet as an EMS service provider; however, there is so much more that defines the clinical quality of an EMS organization, I recommend you identify at least some indicators that your service needs to collect to validate systemwide performance.
Once the data is collected, we can measure and evaluate KPIs by:
- Organization
- Shift
- Service line
- Geography
- Individual crews or practitioners
Displaying KPIs as a dashboard allows you to focus on improving low-performing areas and reinforce high-performing areas.
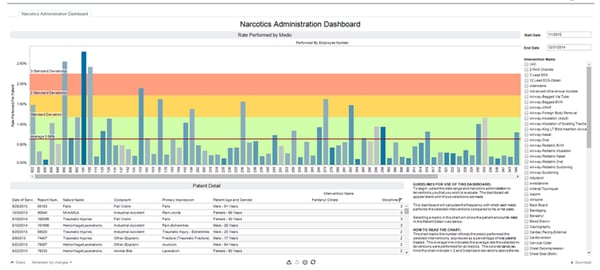
For example, this image from this Insight Analytics dashboard pulls data from ePCR to show which crew member administers which drug to which patients when. This type of tool allows you to compare performance, isolate issues, and address them. Collecting and tracking what matters and seeing it visually is just one of the ways we like to monitor the performance of our crews.
ZOLL: What data do you collect beyond the standard?
Cohen: We use the configurable business logic rules, called closed call rules (CCRs). For any rule that we make, a medic isn’t able to close the chart without filling in the fields. In some instances, what we collect impacts the performance of that call, whereas in others it impacts how a trip gets billed or whether it’s even billable.
Here’s an example of how we put this into practice. A couple of years ago, our medical director wanted to be sure that prior to our medics intubating any patient, we do all of the proper assessments of the difficulty of their airway to make sure that it will have a successful outcome. In many ePCR products, you aren’t able to capture that data. Because our system is configurable, added airway assessment to our system as a mandatory field. As part of our rapid sequence intubation (RSI) rollout, we trained all of our medics in the Difficult Airway Course: EMS™. We found that if medics said they couldn’t intubate, it would be documented as a difficult intubation. If they intubated, they reported it as an easy intubation. To deal with this, we built in a wizard, shown below, that asks our medics to list all the things assessed in order to identify difficult intubations before they potentially harm the airway.
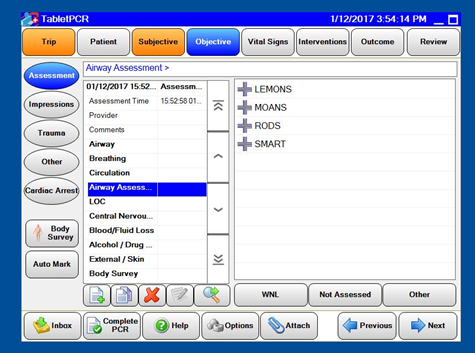
As a result, we’ve seen a high success rate with RSI; 92 percent successful intubations and 98 percent successful airway management (using an alternative device). Here is a snapshot of our performance across the year.
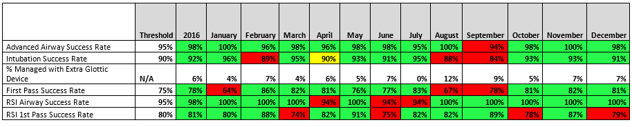
We’ve had no cases where we had to use surgical alternatives for failed airways. And, we are much higher than the national standards, which according to recent publications is between 72 and 87 percent.
ZOLL: What are your closing thoughts?
Cohen: Your ePCR system should be tailorable to the needs of your organization. That ability means your crews can collect the information that’s important to your service. In order to use that data effectively, you need to be able to monitor and analyze it in a simple fashion. The data points you identify should tie back to your goals and metrics of your agency’s strategic plan and help you meet your goals by monitoring them on a real-time basis and give you real-time notifications or indications that you are either underperforming or not performing in a certain area. An organized look at your organization that harnesses our data and highlights what needs our attention is important. Remember, not all ePCRs are the same, and all EMS services are different. It’s important for all EMS services to continue to evaluate how well their data collection and reporting systems ensure it is fulfilling both their clinical and financial goals to remain successful. We believe that going beyond state and national data collection and reporting standards is vital to the success of our organization as we provide EMS service amidst an ever-changing and competitive healthcare landscape.
ZOLL: In part two of the series, we’ll discuss how Cohen uses QA and QI tools to improve clinical performance and billing collection rates.
Related Posts
Inside the App That Cut One Agency’s Charting Time by 85%
News Alert: New ePCR Integration Simplifies EMS Data Management and Enables Better Care Coordination
ZOLL Pulse Blog
Subscribe to our blog and receive quality content that makes your job as an EMS & fire, hospital, or AR professional easier.
ZOLL Pulse Blog
Subscribe to our blog and receive quality content that makes your job as an EMS, fire, hospital, or AR professional easier.