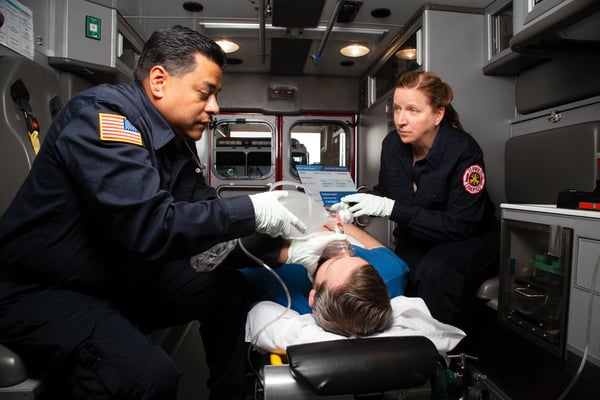
How EMS Technology Integration Can Have Compounding Value for Agencies
Listen to Your Heart: Improving ROSC Rates in EMS
Stories of Survival, Inspiration and Innovation for Heart Month In the past year, ZOLL has hosted several “Outcomes Academy Bootcamps” to educate EMS professionals about the success that organizations such as the Rialto Fire Department has had with a methodology for improving survival from Sudden Cardiac Arrest (SCA)

Stories of Survival, Inspiration and Innovation for Heart Month
In the past year, ZOLL has hosted several “Outcomes Academy Bootcamps” to educate EMS professionals about the success that organizations such as the Rialto Fire Department has had with a methodology for improving survival from Sudden Cardiac Arrest (SCA). After many years and lots of experimentation, Rialto Fire now has a 71% (Utstein) survival rate from sudden cardiac arrest (SCA).

They’ve achieved this by establishing a toolkit comprised of seven components, each one critical to their overall success:
- Continuous uninterrupted compressions utilizing an automated CPR device;
- Apneic oxygenation;
- Use of an impedance threshold device (ITD);
- Using the cot as a tool
- Delaying defibrillation for a certain subset of patient presentations;
- Expanded utilization of waveform capnography; and
- Deprioritizing epinephrine in the order of interventions.
Rialto Fire’s aggressive and proactive approach to Paramedicine has caught the attention of major news publications (JEMs, San Bernardino Sun, etc) as well as the EMS World Expo. The Outcomes Academy was created in an effort to bring Rialto’s insights and methods to EMS organizations across the country and allow them the chance to get hands-on experience and see their cardiac survival toolbox in action.
Last December, Thornton Fire Department hosted one of the Outcomes Academy Bootcamps. Thornton Fire Department is a fire-based EMS delivery system and staffs ALS/Paramedics on all of its units. They run just over 11,000 calls a year with about 80% of those calls being medical in nature. Thornton is the 6th largest city in Colorado with a population of about 140,000 residents. Their fire department delivers suppression, EMS, prevention, public education, and rescue services.
Before and after the Outcomes Academy, Thornton continues to push the boundaries of what they can achieve in improving their ROSC rates. Below, we talk to Theo Gonzales, Safety and Medical Officer at Thornton about their experience learning the Rialto method and implementing it.

Q: When did you first become aware of what Rialto was doing?
A: In 2017 I saw a couple of publications which featured the Rialto Fire Department toolkit for resuscitation.
Q: What were your first reactions?
A: I was really excited. It was inspiring to see someone pushing the envelope of conventional resuscitation methods.
Q: How did you decide to start implementing some of their techniques?
A: Really it was an alignment of the stars so to speak. We are very fortunate to have forward-thinking, progressive leadership. With the support and collaboration of our Fire Chief, EMS Chief, Medical Director and Total Quality Management group, we outlined a plan to improve the cardiac survivability rate in our city.
Q: How did you decide which of the tools in the toolkit to implement, given they are all so important and work in hand in hand?
A: We chose a hybrid approach to implementing some of the techniques in the Rialto toolkit. Working with our medical director we focused on implementing those things that we felt had the most science/research behind them.
We really focused on:
- Apneic oxygenation,
- Uninterrupted compressions,
- Limiting epinephrine doses to 5mg,
- Expanded use of capnography, and
- Extending the total time we actively resuscitate patients.
Our prior benchmarks were BLS airway/BVM immediately and move to intubation after adequate pre-oxygenation. We paused CPR for everything, shocks, pulse checks, intubation.
We gave epinephrine every 3-5 minutes with no maximum – it was not uncommon to give large total doses. We only utilized capnography to confirm intubation success. We would do two rounds of ALS drugs and if no response could terminate resuscitation. 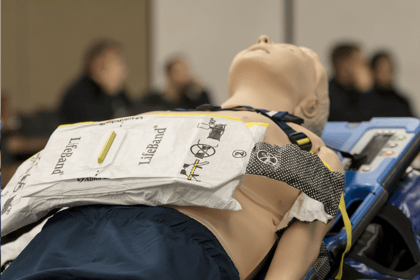
Today, we have added new equipment to support our updated practices. Specifically, we use the ResQPOD®, ZOLL X Series® Monitor with CPR feedback, and the AutoPulse® Resuscitation System.
Q: What were some obstacles you faced? In getting the approval for new techniques, trainings, etc.
A: In reality we have not really faced any obstacles. We haven’t had any problems with trying to push the needle. As an organization, Thornton is really patient centric so the entire team is very focused on patient outcomes. If we can show improvements, then everyone is on board. We get more grief when we are being stagnant than anything!
Our leadership and medical director are committed to being leaders in EMS delivery within our region. With that being said, they are very open to exploring new protocols and equipment to support that vision.
If we had one challenge I would say it truly is the lack of data associated with some of the practices. As more data is compiled we will continue to evaluate the efficacy of adding those practices to our bundle of care. We also continue to look to the horizon for other emerging practices, medications, and equipment.
Q: What have your results been so far?
A: We don’t have a full year of data available yet because we implemented our bundle of care in May of last year. That said, our numbers to date are very promising. We don’t have a complete Utstein update yet, however in 2017 we had just 3 cardiac arrest saves and in 2018 we had 11 cardiac arrest saves. That means, as of this interview, we have effectively tripled our number of cardiac arrest saves.
Q: Have you been able to measure your results and improve again based on what you find out?
A: We constantly evaluate our bundle of care and have a robust total quality management system. We are able to measure our results by utilizing the RescueNet® CaseReview and ESO platforms.
Another big change we made was dispatching an EMS supervisor to every cardiac arrest in the city. In the past, we typically haven’t ever dispatched an EMS supervisor on cardiac arrests. Mainly because we didn’t have any. We are very fortunate to have crews that view having a supervisor on scene as a helpful and encouraging measure. We are there to support the care that citizens receive. Crews also value having immediate access to their CPR report card via the supervisor on scene.
At the conclusion of all arrests a hot wash is conducted and the ZOLL generated CPR performance report is reviewed with the crew. Lastly, our TQM team retrospectively reviews all cardiac arrests for compliance monthly at a meeting which includes our medical director and EMS leadership.
Q: What are your plans for the future? Will you continue to stage out new technique implementations?
A: We have big plans for the future! We are working on several very exciting initiatives that will increase the level of service to the citizens of our community. Specifically, we are keeping our eye on mobile integrated health and intra lipid emulsion therapy in cardiac arrest care.
Again, our eyes are to the horizon for emerging trends in EMS. We will continue to implement new and innovative practices, equipment and medications in the future.
Q: What were your impressions from the Outcomes Academy? Did you find it useful? What did you learn that you didn’t already know?
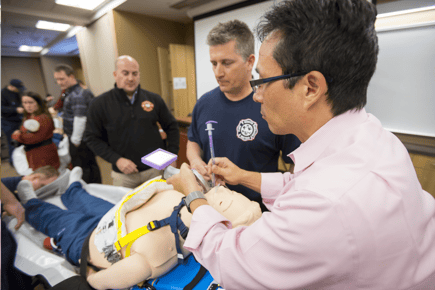
A: I thought the outcomes academy was really well done. I thought it was very useful and thought provoking. I have done a great amount of research on the practices that were presented in the academy so I was familiar with most of the content. What was really impressive was the experience in the practical applications. Such as direct laryngoscopy intubation in the heads-up position.
Related Posts
Inside the App That Cut One Agency’s Charting Time by 85%
News Alert: New ePCR Integration Simplifies EMS Data Management and Enables Better Care Coordination
ZOLL Pulse Blog
Subscribe to our blog and receive quality content that makes your job as an EMS & fire, hospital, or AR professional easier.
ZOLL Pulse Blog
Subscribe to our blog and receive quality content that makes your job as an EMS, fire, hospital, or AR professional easier.