How EMS Technology Integration Can Have Compounding Value for Agencies
Mobile “Interoperable” Healthcare: An Alternative Definition to “MIH”
We’re used to hearing about ‘interoperability’ in terms of communications, but how about its use in information exchange?

We’re used to hearing about ‘interoperability’ in terms of communications, but how about its use in information exchange?

(5 min read) Interoperability is often referenced in the emergency services environment in the context of radios, WiFi connectivity, cellphone reception, and multi-agency communications. It’s why we’ve all transitioned toward 800 MHz radios with state disaster channels ... right?
Entering into our next decade, the term “interoperability” has taken-on somewhat of a new meaning; still focusing on two-way communications, but more so on dynamic information exchange, rather than solely radio traffic.
Health Information Exchange (HIE) has become a new buzzword within the EMS industry, and interoperability is a key driver behind it. Usually where we see interoperability in action is during the time frame of an actual call - but this isn’t where interoperability is stopping!
Device Interoperability
You obtain your first blood pressure manually (which I recommend) and then enter it into your PCR program through your laptop or tablet. Your next blood pressure is obtained automatically via your cardiac monitor and then automatically populated into your PCR via Bluetooth connectivity. That’s device interoperability.
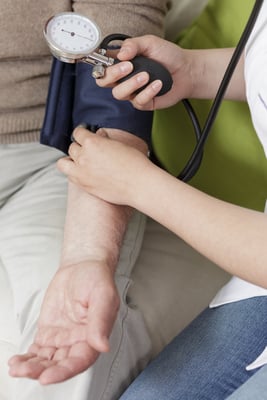
Seamless information exchange is already occurring between devices in the back of your ambulance. We were once primarily concerned with the ability to power our suction units in the back of our ambulances. Now, we’re focusing our (added) attention toward maintaining mobile hot-spots, connecting our devices, and even linking them to multiple platforms all in the effort of becoming more interoperable.
Notifications & Interoperability
Once data has been entered into your PCR software – or onto your smartphone app – it’s now shared with other platforms and individuals. Dispatch and communications centers can track your travel routes for accurate billable miles, and status controllers can track your progress in terms of system status management. Taking this one step further, you’re even able to communicate with your receiving hospital without the click of a radio or even a single phone call being made.
Information from your cardiac monitor can populate into your PCR software, which then connects to an app on your smartphone. This, in turn, is shared through a notification platform that prompts registration, unit clerk, and charge nurse staff at your receiving facility of an incoming patient (including a picture of their drivers’ license, insurance card, most-recent ECG, or even a picture of the vehicle crash that they were just involved in). Once received, facility staff can reply with a confirmation of your communication and can direct you to “room 1” upon your arrival.
Records Management Interoperability
Half of the battle with patient handovers is the reality of the “telephone game.” You tell a nurse part of your handover report, then a physician walks in and you restart (or continue). Afterward, you depart and your patient’s complaint of “syncope” has turned into “nausea & vomiting” with a possibility of a “fall.” Unless you’re leaving a full PCR – including a completed narrative – at the emergency department before you leave the campus, the ED staff may never truly get your full side of the “story.”
Interoperability between PCR and electronic health record (EHR) platforms allows for this information exchange to happen naturally, without continued provider prompts or actions. As soon as you select “complete,” data flows through HIE translators in the form of raw data, and auto-populates into partnering platforms that can upload into communicating platforms for their applications and use. The IV that you started in the field can be auto-populated into the hospital EHR so that it “exists” before the charting nurse even has a chance to enter it. How about your 500 mL of fluids that you administered to your septic patient? It’s already populated into the EHR so that physician orders and sepsis bundles can already account for your recognition and treatment.

Post-Call Interoperability
Beyond the actions & dynamics of an actual call, most of our interoperability has traditionally halted ... until now. This time frame – after the call – is where HIE is taking shape. Two-way automation, integration, and communications are driving post-event interoperability within the healthcare environment. Not only are we seeing pre-hospital information auto-populate into various EHR platforms, but we’re also seeing information exchange in return.
Once registration staff confirm the patient’s identity upon their arrival (remember, you’ve already sent a snapshot of their drivers’ license and insurance card), billing and residence information is compared to your data entries and a billing face sheet immediately populates in your billing service’s inbox. As patient care continues and treatments are ordered, the follow-up component of your patient interaction auto-populates on your patient care dashboard so that you can follow your patient’s diagnosis & disposition in near real-time. Lab results, CT imaging, angiogram snapshots, and updates related to the patient’s admission can all be viewed on a secured platform through your PCR software. This is true information exchange – interoperability – at its best!
We’ve seen a lot of changes within our industry over the past few decades; technology is certainly one of them! We’ve progressed from a purely transport-based industry into one that has become a mobile “interoperable” healthcare profession. There’s certainly more progress to come!
Related Posts
Inside the App That Cut One Agency’s Charting Time by 85%
News Alert: New ePCR Integration Simplifies EMS Data Management and Enables Better Care Coordination
ZOLL Pulse Blog
Subscribe to our blog and receive quality content that makes your job as an EMS & fire, hospital, or AR professional easier.
ZOLL Pulse Blog
Subscribe to our blog and receive quality content that makes your job as an EMS, fire, hospital, or AR professional easier.