How To Cut EMS Patient Collection Time With Digital-first Billing and Payment
Better Care & Billing Metrics Start with ePCR: Part 2
In Part two of this three-part series “Guarantee Your ePCR Works for you, Not Against You”, we asked Steven Cohen, the Assistant Director of EMS at the Jersey City Medical Center EMS Department in New Jersey, to discuss how quality control connects to improvements in key performance indicators (KPIs) such as cardiac arrest outcomes and in reducing the back and forth between billing managers and crew supervisors

In Part two of this three-part series “Guarantee Your ePCR Works for you, Not Against You”, we asked Steven Cohen, the Assistant Director of EMS at the Jersey City Medical Center EMS Department in New Jersey, to discuss how quality control connects to improvements in key performance indicators (KPIs) such as cardiac arrest outcomes and in reducing the back and forth between billing managers and crew supervisors. While measuring the quality of all parts of your patient care delivery may sound daunting, Cohen shares how his operation leverages added ePCR controls and customization to improve outcome measures and billing effectiveness.
Read part one to learn how Cohen’s ePCR system helps his organization achieve their patient care mission of providing great care, while accommodating changing local and national requirements.
ZOLL: Why is quality assurance and improvement a critical part of your operation?
Cohen: At the community level, people want to have the confidence that when they call 911 for a medical emergency, the team that arrives is going to give them the best possible care to allow for the best chances of a successful recovery/outcome. Having robust quality assurance (QA) and quality improvement (QI) program promotes successful outcomes. These outcomes are indicative of the value you provide to your community and health care partners. For example, one measure that is a barometer of how your service can be judged is cardiac arrest survivability: in some EMS systems, survival from ventricular fibrillation cardiac arrest out of hospital can be as high as a 60 to 70 percent, but in other EMS systems, it may be as low as 10 percent or not measured at all. We have taken extra measures through QA and QI within our ePCR to ensure that we accurately track and therefore can improve our survival rates.
ZOLL: How do you use your ePCR for QA/QI?
Cohen: In order to deliver high-performance care at our service, the first thing we did to our ePCR system was to build in a workflow for our QA/QI system. Below is one of our workflows that show how we control which calls are routed to different QI groups based on predetermined criteria. In first level (blue)review, first line supervisors review calls for refusals, which are calls where patients don’t match up with the initial call type. For example, a call may have been advanced life support (ALS), but turned out to be basic life support (BLS).
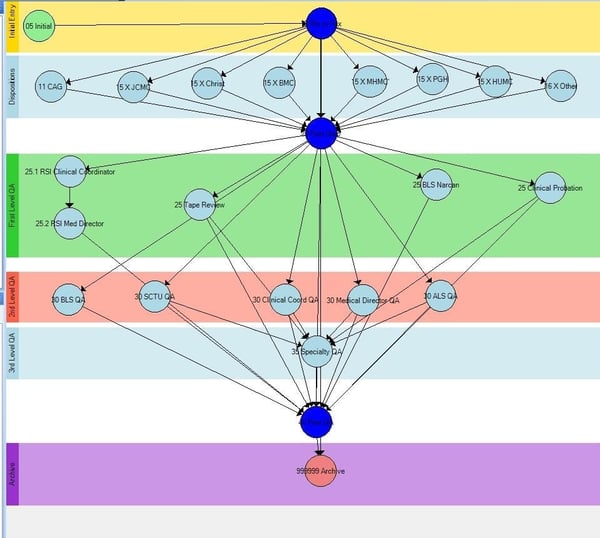
We also configured the system to randomly select 10 percent of the calls for first line review. Specific calls such as cardiac arrest/rapid sequence intubation (RSI) are automatically routed to the clinical coordinator and medical director for review. Calls involving the administration of narcotics for pain control are also routed to our medical director.
ZOLL: How does your QA/QI program translate beyond improving patient care?
Cohen: Through our QA/QI program our crews do two distinct, but related functions. First, they document everything clinical we need to know so we’re always providing high-quality care. Secondly, they collect everything that’s critical around the care process to ensure successful billing for our services. Without the complete chart, you can’t process the bill and create an inefficient process where your billing and patient care departments are in a back and forth struggle just to complete the picture of what happened on a call. Monitoring protocols ensures a higher percentage of calls are billable. We do this through our ePCR system to fully document each of these questions:
- How did the patient get transferred to the ambulance from their house?
- How were they transported in the ambulance; did they sit on the bench seat, in a stretcher or the cab seat?
- How were they taken from the ambulance into the emergency department?
We are able to answer all these questions in each of these different phases through our ePCR and paint a clear picture of both where the patient was and what was happening.
ZOLL: Why is documentation equally important for good patient care and accurate billing?
Cohen: From the patient care aspect, we want to be sure they’re treated properly and weren’t walking to the ambulance with a broken leg or with chest pain. From a billing standpoint, if they’re able to walk, they probably don’t need an ambulance, and we wouldn’t even get paid for that bill. Now from a safety standpoint, we want to be sure patients going from the ambulance to the emergency room (ER) are strapped in on the stretcher. This is important because we’ve noted that when patients try to climb out of ambulances, there’s a much higher incidence of both falls with injuries because it’s such a high step.
The configuration has become part of our culture and daily business. Our ePCR allows us to be sure our protocols are being followed. This gives us the visibility that our crews are both providing and documenting the high-quality care. This level of screening and review helps catch system-wide and individual areas of improvement by having the right experts review our performance.
ZOLL: In part three of the series, Cohen discuss how the Jersey City Medical Center EMS Department has accommodated the needs of their healthcare partners with their patient care documentation system.
Related Posts
How EMS Agencies Can Use Technology To Drive Timely Patient Payments
How EMS Technology Integration Can Have Compounding Value for Agencies
ZOLL Pulse Blog
Subscribe to our blog and receive quality content that makes your job as an EMS & fire, hospital, or AR professional easier.
ZOLL Pulse Blog
Subscribe to our blog and receive quality content that makes your job as an EMS, fire, hospital, or AR professional easier.





