How EMS Technology Integration Can Have Compounding Value for Agencies
Data Says: Switch Out Compressors to Optimize CPR Results
When performing high-quality CPR, one of the most important factors is compressor fatigue

When performing high-quality CPR, one of the most important factors is compressor fatigue. When I started in EMS, the person with the most experience did the compressions the entire time. Six years ago, we finally stopped this time-honored tradition that didn’t serve our patients the way it should have. Data and evidence show that compressions are now one of the biggest factors in survival. If the person doing the compressions is unable to deliver the proper rate and depth, bring in a fresh compressor every two minutes.
Analyze Your CPR DeliveryWith the use of RescueNet CaseReview, ZOLL’s software design to help you analyze the complete resuscitation event, we can see how CPR quality diminishes quickly, even though the crews believed they weren’t tired and still delivering high-quality CPR. Let’s take a look at the data to see how a crew that used only one compressor actually performed:
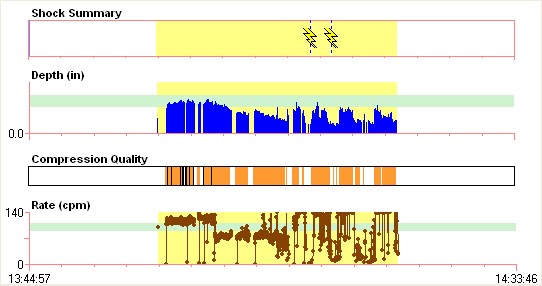
Depth. Look in the “Depth (in)” area. The light green strip near the top is our target range for our agency of 2.0 to 3.5 inches. Each blue line is one compression. Tightly compacted blue lines means there were no measurable pauses between compressions. Notice the first round (two minutes) of CPR is in the target and then the depth diminishes in the middle of the second round. This was about the three-minute mark. In the graph below you can see that the Edelson study found that the deeper the compression, the better the shock success. This graph is in millimeters, so 50 millimeters is about two inches. We hope everyone is practicing the American Heart Association (AHA) 2015 Guidelines for compression depth and pushing at least two inches for adults. We aim for 2.5 inches, but want no less than 2 inches.
Rate. Take a look in the “Rate (cpm)” box in the code review above. The green strip in this box is our target rate of 90 – 110. Each brown dot is one compression. You can see this compressor started out a little on the fast side. Faster is better than slower, but many of the compressions are still out of the target range. This issue would have been brought up in a QA review with the crew. Notice as the compressor starts to fatigue, the rate goes all over the place. To make up for a shallow depth, most compressors will try to increase their rate. Please remember, a faster rate doesn’t make up for a shallow depth. These two components have to be within range to give your patient the best chance of survival.
What if You Don’t Have Real-Time CPR Feedback?
You are now aware that compressor fatigue is a real thing. Performance diminishes well before the compressor notices they are becoming fatigued. Be meticulous with your CPR performance – practice, practice, practice and then practice some more. Consider incorporating the pit crew method into your training, where resuscitation teams focus on the person doing compressions so they can concentrate on each component of CPR – rate, depth and minimizing any unnecessary pauses. Pit crews in auto racing perform with amazing precision and are able to accomplish amazing things. Everyone on the team has a specific job to do and everyone supports the other members without getting in their way. We can use this methodology in managing a cardiac arrest scene. It can be easily adapted to whatever your crew make-up, defibrillator equipment or CPR method. It can be used with a two- or four-person crew and as other help arrives, can easily incorporate more members. And require your crews to switch compressors every two minutes to deliver optimal CPR. Your patients will thank you!
Related Posts
Inside the App That Cut One Agency’s Charting Time by 85%
News Alert: New ePCR Integration Simplifies EMS Data Management and Enables Better Care Coordination
ZOLL Pulse Blog
Subscribe to our blog and receive quality content that makes your job as an EMS & fire, hospital, or AR professional easier.
ZOLL Pulse Blog
Subscribe to our blog and receive quality content that makes your job as an EMS, fire, hospital, or AR professional easier.