Meet the New ZOLL Dispatch and ZOLL Respond CAD Solution
MISSION: INTEROPERABILITY: PART 1
(5 min read) What if I were to tell you there is a pill you can prescribe to prevent death related to sudden cardiac and stroke?

(5 min read) What if I were to tell you there is a pill you can prescribe to prevent death related to sudden cardiac and stroke?
Every day I interact with paramedics, fire fighters, doctors, healthcare providers and professionals involved in the chain of care and on the front lines combating death. I see them diligently providing excellent care to the people in their charge and working long hard hours helping to safeguard their communities. I like to think the role I play helps them.

My father is a victim of both stroke and cardiac arrest. My stepmother a stroke survivor. I have a wife and two children who could be at risk of either of these sentinel events within our lifetime. I think about it every day, as I imagine many of you must. What can I do to protect them? What might we all do to help cure our population?
I dare to believe we can end death from sudden cardiac arrest and stroke within our children’s lifetime.
Why?
For one reason, my undergraduate institution was a chief participant in a nationwide, federally funded, study of the human genome, also known as the Human Genome Project. As a result, I’ve had classmates who discovered and eradicated cancer genes.
Another reason: I work for one of the largest medical technology and resuscitation companies in the world. My employer holds medical patents and has invented technology to bring patients back from the brink of cardiac death. And they do a fantastic job of providing continuing education on medical and technological advances.
My optimism is backed by science. There is a fair bit of research, studies, and data points collected which support my belief that a cure may very well be in our grasp. But I also believe this based on first-hand experience. In the aftermath of my dad and stepmom’s sentinel events, there was a decent amount of data available to me to study. What I observed and collected following these events would probably shock you, including missed medical opportunities that would’ve improved their chances of survival.
What I’m about to suggest might sound a bit radical, but if I’m right I would give this cure away for free.
You see, the pill that was mentioned in the opening sentence is not a pill we will prescribe patients. Rather this is a “pill” that care providers must administer to themselves, daily.
The key to a successful outcome in Cardiac Arrest, Stroke, STEMI, or any other time-dependent illness or injury is “action” with a focus on “how” things are done. The failure to act and provide care when and where needed, including getting the patient to the appropriate destination in the appropriate time is critical to survival.
For a patient in Cardiac Arrest, administering great CPR is hard. If you do not definitively know the rate and depth of your compression, you cannot perform high quality CPR. You have to know precisely “how” fast and “how” hard to push, for this intervention to be successful. Achieving and maintaining high quality CPR is almost impossible without some form of real time CPR feedback that is available today.
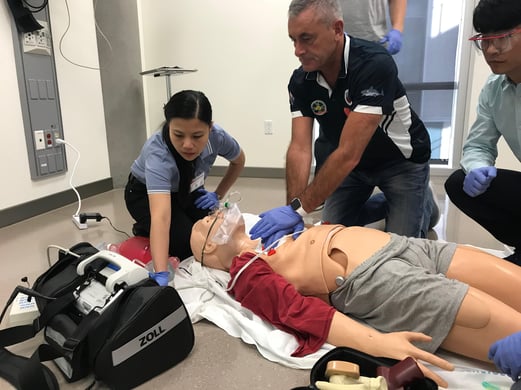
Acute Stroke patients also require the same attention to detail to rapidly identify a stroke and transport the patient to the appropriate Stroke Center within a very narrow treatment time window. Data published by the Centers for Disease Control and Prevention highlight:
- “In one survey, most respondents—93%—recognized sudden numbness on one side as a symptom of stroke. Only 38% were aware of all major symptoms and knew to call 9-1-1 when someone was having a stroke.
- Patients who arrive at the emergency room within 3 hours of their first symptoms often have less disability 3 months after a stroke than those who received delayed care.”
Unfortunately, many that suffer from a stroke are found hours after their symptoms began and are outside the window for therapeutic treatment. Stroke care cannot improve without rapid detection, accurate measurement, and Integrated Systems of Care.
New technology, predictive modeling, and protocols will be key to the future of improved outcomes, but how should local EMS and regional Systems of Care integrate these tools? Most of these tools either require or are much more effective when they are integrated or interoperable across each patient’s multiple healthcare providers (EMS, hospital, physicians, etc.). Understanding, this must be done securely, based on current HIPAA and other patient-centered privacy requirements. HIPAA should never be a reason for this critical integration and interoperability to fail.
Integration and interoperability are critical to quality care and each patient’s outcome. Key patient information including medications, allergies, past medical history, and insurance network demographics must be accessible at the time of care.
Within EMS, some estimate that over 90% of patient records in the country are still transmitted to the hospital via fax machine. Of all the EMS records faxed to the hospital prior to patient arrival, A lack of integration and interoperability inevitably leads to a poor patient experience (outcomes and satisfaction), a negative impact on our community’s health, and higher healthcare costs: The Triple Aim.
The Institute for Healthcare Improvement’s (IHI) Triple Aim which has recently been revised in favor of the Quadruple Aim is a critical concept driving the future of healthcare.
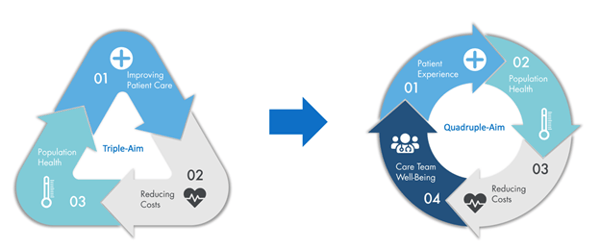
To some degree, this is a “chicken vs egg” dilemma. Is it integration and interoperability that drives the Quadruple Aim? Or vice versa… Learn more in part 2 of Nick Sortin’s Mission: Interoperability.
Acknowledgement:
The author is extremely grateful and sincerely acknowledges the guidance and help in editing from Dr. Greg Mears, Medical Director at ZOLL.
Related Posts
Collect More Revenue Faster: The Pivotal Role of Clear, Concise, and Complete Documentation
ZOLL Pulse Blog
Subscribe to our blog and receive quality content that makes your job as an EMS & fire, hospital, or AR professional easier.
ZOLL Pulse Blog
Subscribe to our blog and receive quality content that makes your job as an EMS, fire, hospital, or AR professional easier.




