Meet the New ZOLL Dispatch and ZOLL Respond CAD Solution
MISSION: INTEROPERABILITY: PART 2
(4 min read) Part 2

(4 min read) Part 2. If you missed Part 1, you can read it here.
In Part 1, I posed a question: what if I were to tell you there is a pill you can prescribe to help prevent death related to sudden cardiac arrest and stroke?
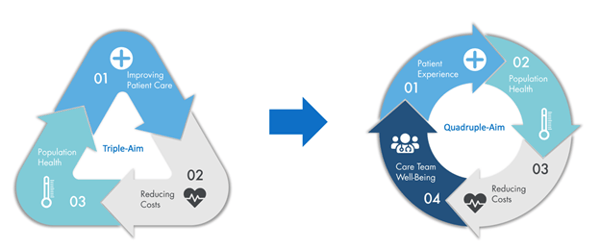
I touched on the role of timely detection and interventions in improving cardiac and stroke outcomes. I highlighted improvements in technology – devices that can accurately assess CPR quality, affordable wearable devices that can measure vitals in real time – that produce a treasure-trove of data for clinicians and care providers. I identified the need to make accurate patient information available to all providers at the time of care, and touched on how all these factors relate to the Quadruple Aim.
Now I’d like to propose my cure, a prescription you can incorporate into your skills training and protocols to drastically improve patient outcomes.

The pill I’m asking providers to swallow is Interoperability. No more centralized systems of record and silos of care, no more data hoarding. Progress in achieving the goals of the Quadruple Gain will only come after embracing the principal of health data interoperability. Specifically, holistic structural and foundational interoperability as defined by the Health Information Management Systems Society (HiMSS).
I share the HiMSS vision statement: “A world where everyone, everywhere, has access to a health and wellness ecosystem that works - one with the human at its heart.”
It must begin with an understanding that patient data belongs to the patient. It is their story, one that must evolve and travel with them across all systems of care throughout their life. It will be their family’s record after they are gone.
Getting to this cure will require both commitment and investment on your part. Implementing technologies architected around core principals of interoperability, providing immediate availability of critical information, and developing intrinsically safe data practices are all necessary steps towards meaningful interoperability.
Making the investment now not only moves us all closer to the goals of the Quadruple Aim, it also improves the viability of your organization as models and systems of care continue to evolve. Continuous improvement will be the single heaviest weighted factor going forward governing standards for reimbursement in healthcare and advancing population health. New landscapes of care are developing, and models like the “Treat, Triage, or Transport” (ET3) program will require improved communication between field personnel and providers/facilities.
Get ahead of these shifts and take a critical look at your policy for medical communication. Will your system need to leverage shared documents, vitals, text, talk, or video? Providers who fail to make progress toward interoperability increasingly put both their business and their patients at risk.
Borrowing from the IHI, I am inspired to suggest a multi-pronged mission. I propose the aims of interoperability must maintain the decentralized patient system of record and be simultaneously:
Accurate
Immediate
Ubiquitous
Agnostic, and
Intrinsically Safe
I think even most layman can accept at first glance accurate and immediate information is a necessary standard for health care records. Ubiquitous, on the other hand, may cause concern for some; to those I’d invite you to consider that secure is not necessarily safe for the patient. If there is a barrier to data access that delays a vital intervention, the propensity to harm the patient is increased.
Our data sources and care systems must be agnostic so that the best information for the patient and provider from all possible sources is available irrespective of origin or platform. Intrinsically safe, meaning information and architecture authored and stored securely from the point of creation.
My proposed cure encompasses a vision of interoperability that is attainable: enable a real time 360-degree view of a patient’s health, allow clinicians to make faster more informed decisions, leverage software models and predictive algorithms to detect life-threatening events hours or even days before they happen. This vision will become reality only if we remain committed, if we do not accept data silos and closed systems as the norm, if we push for systems “with the human at their heart.”
It is not MISSION:IMPOSSIBLE as long as we commit to take measured steps to develop this cure together. Ensure you are treating information collection and delivery as a line of patient care in and of itself. If we are to accomplish the goals of the Quadruple Aim, if we are to see an end to deaths resulting from stroke and sudden cardiac arrests within our lifetime, it is imperative all healthcare professionals take this pill and take up the mantle MISSION: INTEROPERABILITY.
Acknowledgement:
The author is extremely grateful and sincerely acknowledges the guidance and help in editing from Rob Humphreys, Senior Product Manager for ZOLL Online.
Related Posts
Collect More Revenue Faster: The Pivotal Role of Clear, Concise, and Complete Documentation
ZOLL Pulse Blog
Subscribe to our blog and receive quality content that makes your job as an EMS & fire, hospital, or AR professional easier.
ZOLL Pulse Blog
Subscribe to our blog and receive quality content that makes your job as an EMS, fire, hospital, or AR professional easier.




