What Does Hospital Data & HIE Really Mean to EMS? Part 2 of a 3 Part Series
Welcome to part two of a three-part series focusing on healthcare reform and the future of Emergency Medical Services (EMS)
Welcome to part two of a three-part series focusing on healthcare reform and the future of Emergency Medical Services (EMS). Last month, we reviewed the key concepts of healthcare reform, including the Triple Aim. This month we will focus specifically on Health Information Exchange (HIE) and 4 key EMS use cases where HIE directly impacts operational and patient outcomes. I will also touch on a new state Medicaid funding opportunity for EMS and HIE. Next month, we will finish up this series with a vision of the future.
The Future of EMS
Healthcare reform will bring significant and meaningful improvements to EMS. To achieve the Triple Aim of improved patient satisfaction (experience and outcome), improved population health (public health and prevention), all while controlling/decreasing cost, EMS must integrate with the healthcare system. Traditional EMS will be a key decision maker for each healthcare system’s success. Since each community typically has 2 or more healthcare systems (hospitals and outpatient systems), it is critical to make sure each patient stays within their healthcare system, to assure continuity, efficiency, and positive outcomes. Through effective EMS patient navigation, the patient not only lands in the correct healthcare system but also enters it through the most appropriate way. Less than one-third of EMS transports require the Emergency Department. EMS treatment and referral to a clinic (at a later date) or transportation to an alternative destination (clinic) will be normal in future.
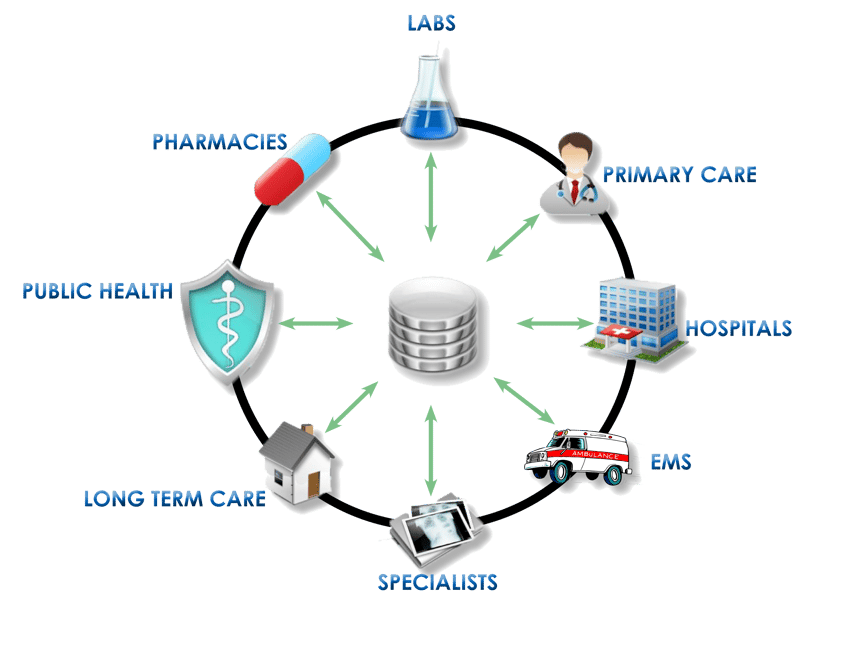
The Exchange of Electronic Patient Data Between Hospitals & EMS
For EMS to successfully make the correct patient navigation, on-scene treatment, and destination decisions, timely access to the patient’s medical information is critical. Health Information Exchange allows healthcare professionals and patients to appropriately access and securely share a patient’s vital medical information electronically.
The Office of the National Coordinator for Health Information Technology (ONC) has established requirements for the exchange of electronic health records. This is often referred to as Search, Alert, File, and Reconcile. From an EMS perspective, these terms can be defined as follows:

- Search is the ability to search across healthcare systems for a patient’s individual health record. This could include information on their medical history, medications, allergies, and end-of-life decisions. This information should be accessible in the Dispatch Center as well as at the location of the patient and/or the EMS event.
- Alert is the ability to notify the receiving hospital or the patient’s healthcare provider of the patient’s condition and status. For an emergent event, such as a STEMI, significant trauma, or Stroke, this alert would activate the appropriate hospital assuring they are prepared, when EMS arrives, to deliver the time-dependent definitive care that the patient requires.
- File is the ability for EMS to create an electronic health record (EHR) representing the EMS service delivery and care associated with the patient event. This EHR should contain structured data that can be electronically transmitted to the receiving facility and the patient’s healthcare provider. This allows the patient to have an integrated longitudinal documentation of their healthcare.
- Reconcile is the ability for EMS to obtain key EHR content such as diagnosis, disposition, billing, and outcome information from the patient’s EHR after the event. This is critical to EMS business, service delivery, quality management, and outcome measurement.
How to Fund for Search, Alert, File & Reconcile Capability for EMS
Hospitals and physician’s offices have received federal funding over the past several years to implement EHR systems. Currently, over 98% of Hospitals have EHRs and over 80% are exchanging health information with outside providers.
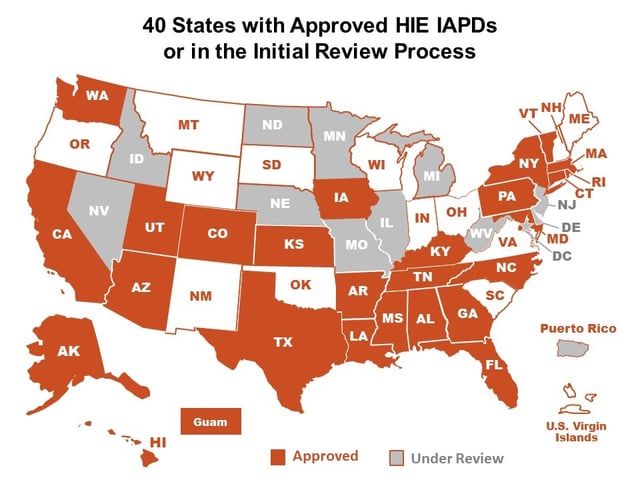
EMS unfortunately was left out of these original funding initiatives and EMS data systems are now working to build the full Search, Alert, File, and Reconcile capability. Recently a Federal/State (90%/10%) Medicaid Match funding opportunity was introduced to EMS. Funding through this program is available until 2021. It’s focus in on implementing health information exchange and interoperability. The program is managed through each state’s Medicaid office but not all states are participating. The map below outlines each states current participation status. Even if your state is not listed as a participant, please contact your state’s Medicaid office, as their status may have changed. This is a great funding opportunity for EMS.
Next month, we will explore how healthcare reform, the Triple Aim, and HIE ultimately will change EMS forever. Data, along with the devices that collect and analyze it, were once tools in our tool belt used as needed in the provision of patient care. Data and devices now are much more than that...they are a member of our healthcare team. They provide information, guidance, insight, and a level of intelligence directly connected to positive outcomes.
Related Posts
ZOLL Pulse Blog
Subscribe to our blog and receive quality content that makes your job as an EMS & fire, hospital, or AR professional easier.
ZOLL Pulse Blog
Subscribe to our blog and receive quality content that makes your job as an EMS, fire, hospital, or AR professional easier.




